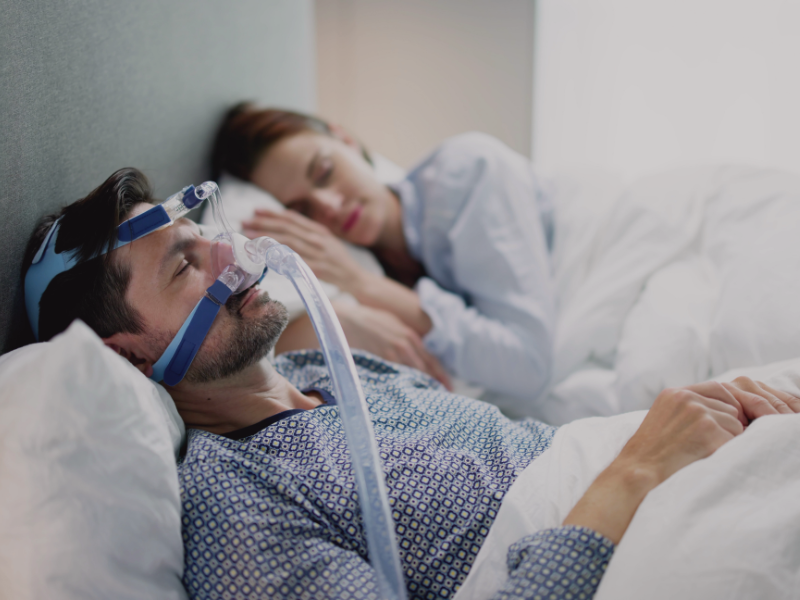
Obstructive sleep apnoea (OSA) is a potentially serious sleep disorder. OSA occurs when your throat muscles intermittently relax and block your airway during sleep.
This may lead to regularly interrupted sleep, which can have a big impact on quality of life and increase the risk of developing certain conditions. During an episode, the lack of oxygen triggers your brain to pull you out of deep sleep – either to a lighter sleep or even wake you. This allows your airway to reopen and you are therefore able to breathe normally.
Common symptoms of OSA can include loud snoring, noisy and laboured breathing, repeated short periods where breathing is interrupted by gasping or snorting.
We put a few questions to our very own Clinical Director, Shaw Somers to find out more about this disorder, it’s links with obesity and treatments.
What is obstructive sleep apnoea and is it serious?
‘This is essentially pathological snoring! The breathing becomes so difficult during sleep that blood oxygen levels drop and the body becomes distressed. This is why sufferers feel awful after night’s sleep and can start to become chronically sleep deprived and ill.’
Why is OSA linked to obesity?
‘As the body gains weight the neck thickens and the breathing pipes become more easily collapsed.’
What treatments are there?
‘One of the most effective ways to treat the disorder is a Continuous positive airway pressure (CPAP) device. Aside from losing weight, only pressured air can keep the breathing path open- hence the machine!
‘The machine works by blowing air into the lungs each time you breath in.’
Many of our past patients have had to use a CPAP device; we caught up with a few to hear more about their experience.
Here is what Tracey had to say; ‘ I was on a CPAP for two years prior to my Bypass surgery. I gave my machine back 20 weeks after the procedure.
‘My sleep is amazing. I no longer stop breathing. I do have other issues that interrupt my sleep but thanks to weight loss surgery sleep apnoea is no longer one of them!’
Learn more about Tracey’s full weight loss surgery.
Another past patient, Kim told us, ‘I handed min back 6 months after surgery. It would have been sooner but I had to wait for an appointment. It’s great to cross off another comorbidity.’
If you think you might have OSA it is important to seek advice from your GP.